|
| |
Breastfeeding
Health Basics: A supplement to Issue no. 37 - June 1989
pdf
 version of
this Issue version of
this Issue
|
There is much information in this issue that is valuable
and useful. Online readers are reminded, however, that treatment guidelines and health
care practices change over time. If you are in doubt, please refer to
WHO's up-to-date Dehydration Treatment
Plans.
|
Pages 1-6 Breastfeeding
A supplement to Dialogue on Diarrhoea Online
Issue 37 - June 1989
|
DDOnline Breastfeeding
supplement to DD37  Page 1 2
Page 1 2
HEALTH BASICS
BREASTFEEDING
Breastfeeding is the best way to feed a new baby: breastmilk is the perfect food for
babies, and breastfeeding is safer and cheaper than any milk which can be bought. Babies
fed from the breast are more likely to be healthy and free from diarrhoeal diseases. Why breastfeed?
|
Breast is best - nothing that money can buy is as good for a
baby as breastfeeding
- Breastmilk is the best food there is for babies: it provides all the goodness and energy
needed for healthy growth, and is easier for the baby to digest than any other milk
- Breastfeeding passes on protection from mother to baby against infections; breastmilk is
the only milk which contains antibodies to fight diseases such as diarrhoea (bottle-fed
babies do not get this protection)
- Breastfeeding is cleaner and safer than giving milk from a bottle or other container
which can be easily contaminated with dirt and germs
|
 |
- Breastmilk is much cheaper than powdered milk food - all it costs the family is the
little extra food needed by the mother. Special baby foods and milk formulae are very
expensive and never as good as breastmilk
- Breastfeeding does not use up valuable fuel and water resources which may have to be
gathered or bought and used to boil water for bottle-feeds, and to ensure that feeding
bottles and teats are sterilised
- Breastfeeding is convenient: it can be done whenever the baby is hungry or unhappy, at
any time of the day or night. Breastmilk is always available at the right temperature and
never goes bad
- If a mother is breastfeeding a baby frequently by day and night, she is less likely to
become pregnant again during this time
- Breastfeeding helps to stop maternal bleeding after delivery
- Breastfeeding helps to develop the emotional bond between mother and child
Why does breastfeeding need to be promoted? Most women know that breastfeeding is the natural and best way to feed a baby, but
there are many pressures on them not to breastfeed. Traditionally, women have always
breastfed: they have seen other babies breastfed and learnt from their mothers and other
women in the community. But, increasingly, women are being told that bottle-feeding is the
modern way to feed a baby, and must therefore be better. Artificial babymilks are
sometimes promoted very aggressively and are even provided in hospitals. Once a mother
starts to give milk formula, and stops breastfeeding, it is difficult for her to start
breastfeeding again. Women need to feel confident that they can provide the best food for their own babies.
Health workers can encourage and support mothers, providing information and practical
advice about breastfeeding. This information is not new but, often, it needs to be
re-learnt in modern urban communities, especially when mothers are working outside the
home, when they have moved away from their extended family, or if they give birth in
hospital.
|
|
DDOnline Breastfeeding
supplement to DD37  1 Page 2 3 1 Page 2 3
Successful breastfeeding Before the birth
- Tell women about the advantages of breastfeeding
- Discuss how they fed previous children, and reassure them that difficulties can be
overcome
- Explain what to expect as they start to breastfeed
- Examine the breasts and nipples - reassure women who think that their nipples are flat
or short that a baby feeds from the breast and the shape of the nipple is not important
- Encourage the mother to eat an adequate mixed diet so that her baby is not too small and
her body builds up stores of fat and other tissues which will be used to make milk after
the baby is born
After the baby is born
|
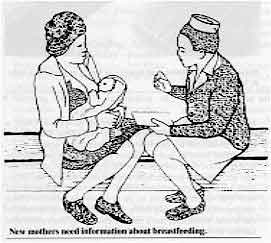
New
mothers need information about breastfeeding.
- The baby should be given to the mother to hold as soon as s/he is born, and she should
put the baby straight to the breast. After a normal delivery, most babies want to suck
during the first hour after they are born. This is a good time for the baby to learn to
suck, and it is important to establish the bond between mother and baby
|
 |
- It is important that the baby gets the first breastmilk (called
colostrum) because it
gives protection against infection. Colostrum is thicker and yellower than later milk, and
it comes only in small amounts in the first few days after delivery. Colostrum is all the
food needed at this time - no supplements are necessary, not even water or glucose water.
A baby is born with enough water in its body to last several days if necessary. Many
babies lose a little weight in the first week, but this is normal
- It is important that the baby learns to suck in a good position - s/he must take enough
of the breast into the mouth so that the tongue can express the milk from beneath the
areola
- Breastfeed as often as the baby wants to - frequent suckling helps to make more milk,
and helps to prevent problems like engorgement (breasts which are swollen and painful)
- Each feed should continue for as long as the baby wants to suck; when s/he has finished,
s/he will release the nipple spontaneously. A baby should never be pulled off the breast
suddenly (if a mother has to stop in the middle of a breastfeed for any reason, she should
gently put her finger into the baby's mouth so that it releases the breast)
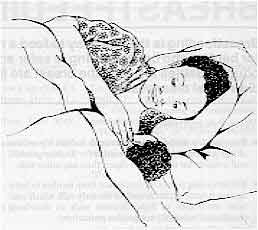
It is quite safe for mother and baby to sleep together, and
night feeding is easier.
- Even in hospital, a mother and baby should sleep in the same bed, or together in the
same room, so that feeding is not restricted in any way. If a baby sleeps with its mother,
night feeding can go on without the mother having to wake up or be disturbed more than
necessary (the baby will not be crushed by the mother unless she is very ill or drunk or
sedated)
|
 |
- Let the baby finish sucking from the first breast, and then offer the other side. Some
babies do not want milk from the second side. Do not try to make them take both sides, or
they may take more than they need. But it is important to start from the other side next
time, to keep the milk flowing. When the baby is bigger, s/he will probably need both
sides
- Breastmilk is always the best food for a baby - if a mother is unable to breastfeed her
own baby, expressed breastmilk, or breastfeeding by another mother is better than formula
milk
- In the first four to six months of life, breastmilk provides all the food and drink a
baby needs - do not give anything else
|
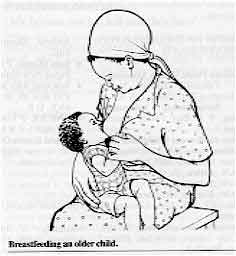
Breastfeeding an older child.
- When a baby is ready for other foods, breastfeeding is still important and should
continue until the baby is at least two years old; breastmilk can still provide a third of
all the energy and protein a child needs during the second year of life
- When you decide to stop breastfeeding do it slowly over a period of time; comfort the
child and make him or her feel loved in other ways
|
 |
|
|
DDOnline Breastfeeding
supplement to DD37  2 Page 3 4 2 Page 3 4
How to help Mothers of new babies need support and help. They need confidence that they can
breastfeed. Reassure mothers who worry about not being able to provide enough milk for
their babies. Health workers can provide support and information, as well as helping with
problems or sickness. But everyone in the community can help a breastfeeding mother in
some way.
- Other members of the family can help with household tasks and make sure that the mother
gets enough to eat and enough time for her baby
- If a woman has to be away from her baby at any time, she can express milk into a clean
cup for a helper to feed to the baby while she is away
- Other members of the family can also help to look after any other young children and
stop them from feeling left out
- Older women can provide special help and advice from their own experiences of
breastfeeding, and help new mothers not to feel embarrassed about breastfeeding
|
Positioning the baby at the breast
It
is important to put a baby onto the breast in the right position. If the baby does not
take enough of the breast into his or her mouth, so that s/he sucks on the nipple, it
causes pain and damages the nipple, and the baby does not get the milk efficiently.
- Hold the baby close. facing the breast
- Offer the whole breast. not just the nipple, to the baby
- Wait until the baby's mouth is wide open and move him or her quickly onto the breast so
that s/he takes a good mouthful. S/he should come onto the nipple from below it, not from
on top
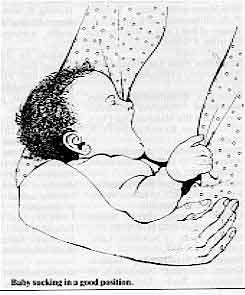
Baby sucking in a good position.
A baby in a good position:
- is close to the mother, and the chin touches the breast
- has the mouth wide open
- the lower lip has turned out (and you may be able to see the tongue)
- takes slow, deep sucks
- causes no pain to the mother
|
 |
|
|
DDOnline Breastfeeding
supplement to DD37  3 Page 4 5 3 Page 4 5
|
Expressing breast milk If a mother
cannot take her baby with her to breastfeed at work, she can express her milk by hand
before she goes to work, and leave it for a helper to feed to the baby while she is away.
If a mother also expresses milk while she is at work, this helps to keep up her milk
supply.
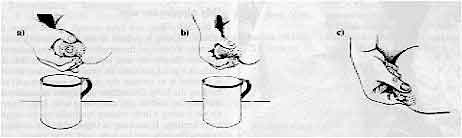
- Express milk into a clean cup or container. To make sure the cup is clean wash it with
soap and water and leave it to dry in the sun; then pour boiling water into the cup. The
sun and boiling water will kill most germs.
- Wash hands thoroughly with soap before expressing milk
- Lean forward, supporting the breast over the cup or bowl
- With thumb above and first finger below the nipple, press in towards the body a little
way (a)
- Then bring thumb and finger together, squeezing behind the nipple (b)
- Release and repeat until milk starts to drip or flow
- Press the areola (the darker area around the nipple) to the left and right of the nipple
in the same way, to make sure that milk is expressed from all sectors of the breast (c)
- Expressed breastmilk (EBM) should be given to the baby from a clean cup. Feeding bottles
should not be used because they are very hard to keep clean and because they make the baby
less eager to suck at the breast
- EBM can be stored during the day (up to six hours if no refrigerator is available, and
up to 24 hours if kept refrigerated), but it should be kept covered and as cool as
possible. Do not worry if the milk separates; it can be shaken up and is still good to use
- Using EBM is the best way to feed a baby who is too ill to suck, and expressing milk can
relieve very full or leaking breasts
|
|
Breastfeeding and diarrhoea
- Babies who are exclusively breastfed are less likely to get diarrhoea, because
breastmilk is free from germs and contains antibodies which protect a baby from infection
|
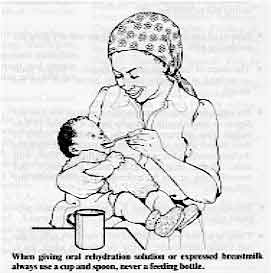
When giving oral rehydration solution or expressed breastmilk
germs always use a cup and spoon, never a feeding bottle.
- Bottle-fed babies are more likely to get diarrhoea. Feeding bottles are very difficult
to keep clean, and dirty bottles are a major source of illness, especially diarrhoea;
bottle-fed babies are also at risk from contaminated water which may be used to mix up
powdered milk
|
 |
- If a baby has diarrhoea, always continue breastfeeding because a baby still needs food,
and especially liquids, to replace what is lost during the diarrhoea. Breastfeeding will
also reduce the stool volume and speed recovery
- When a baby has frequent diarrhoea, oral rehydration fluids may be needed as well. These
should be given by cup and spoon. If the baby is too weak to suck at the breast, expressed
breastmilk can also be be given by cup
- Cups used to feed a baby with expressed breastmilk should be carefully washed with
boiled water to remove germs
|
|
DDOnline Breastfeeding
supplement to DD37  4 Page 5 6 4 Page 5 6
Facts about breastfeeding
- Almost every mother can breastfeed - probably less than one in every hundred cannot
|
Being able to breastfeed often keeps up the supply of milk.
- Malnourished women can breastfeed, and the quality of their milk is still good. If they
are severely malnourished, they may produce a smaller amount of milk. However, if a woman
is undernourished, the milk is made at the expense of her own body tissues, and she may
lose weight and have less strength and energy. So it is important for a breastfeeding
woman to eat enough to remain strong and healthy herself
|
 |
- Breasts of any size (large or small) are equally good for producing milk
- The shape of the nipple does not matter - long or short - as long as the baby takes the
breast well into the mouth
- Breastfeeding does not mean that a woman will lose her figure - breastfeeding actually
helps a woman to lose weight after pregnancy, and the breasts will return to their former
shape after weaning, provided she supports the breasts with a bra or binder when they are
heavy with milk. (Some changes occur with pregnancy, and breastfeeding or not
breastfeeding does not make any difference)
- Breastfeeding can continue if a woman becomes pregnant again
- There is no bad medical effect on a mother's milk if she has sexual intercourse during
the months when she is breastfeeding
|
Problem solving
'My breasts are too full and
they hurt'
When the milk first comes in to the breasts, they may feel hard and swollen and
painfully full. This is called engorgement, and if engorgement persists it can be relieved
by expressing milk from the breasts. The best way to prevent engorgement is to let the
baby suck as often and as soon after birth as possible.
'My nipples are sore'
If the baby does not take enough of the breast into the mouth, sucking is painful. If
the baby continues to suck in this way, it damages the nipple skin and may cause cracks or
fissures. To prevent sore nipples, make sure that the baby sucks in a good position. To
treat sore nipples, often all that is needed is to correct the sucking position and
continue feeding the baby. Do not put ointments or antiseptics onto the nipples, and do
not wash them with soap. Exposure to air, or leaving a little creamy hindmilk on the
nipples may help healing. If sucking is impossible for a day or two, express the milk and
feed the baby from a cup.
'My baby refuses/finds it difficult to breastfeed'
Occasionally a baby who refuses to suck is seriously ill (e. g. with neonatal tetanus,
or an infection) so check his or her general health first and get help if you are worried.
Babies may refuse the breast if they have been fed from a bottle or fed in a poor position
so that they do not get the milk efficiently, or if they have been separated from their
mothers. Usually the problem is simple: the baby may have a blocked nose, which can be
cleared before each feed with the tip of a clean cloth. Check also for thrush or other
sores in the baby's mouth. A very small baby may find it difficult to suck, and should be
fed expressed breastmilk by cup until strong enough to take the breast.
'There is a painful swelling in my breast'
The tubes or ducts which carry milk through the breast may sometimes become blocked
causing painful swellings and sometimes infections. To prevent infection, the lump should
be gently massaged towards the nipple to unblock the duct, and unrestricted breastfeeding
should continue. Feeding should be started with the affected breast for a few days, if
possible, to make sure that this breast is emptied.
'I do not have enough milk'
This is the most common reason mothers give for stopping breastfeeding or early
supplementation with formula milk. Usually a mother does have enough milk, but needs to be
reassured and encouraged. A baby is taking enough milk if s/he gains 125g or more in
weight each week, and urinates at least six times a day, with clear or light yellow urine.
More frequent breastfeeding usually results in increased milk production. Sometimes the
baby is feeding too often anyway and that is why the mother thinks she does not have
enough milk.
- check feeding pattern:
if infrequent, feed more often, stop supplements, bottles etc.
- check feeding position:
if poor, correct and then build up milk
|
|
DDOnline Breastfeeding
supplement to DD37  5 Page 6 5 Page 6
Addresses for organisations supplying
books, manuals, audiovisuals and newsletters are listed under sources of information and
materials. SOURCES OF INFORMATION AND MATERIALS
- American Public Health Association. 1015 Fifteenth Street, N W, Washington, D C
20005, USA.
- The Breastfeeding Information Group. P O Box 59436, Nairobi, Kenya.
- Center to Prevent Childhood Malnutrition. Suite 204, 7200 Wisconsin Avenue,
Bethesda, MD 20814, U S A.
- IBFAN Africa P O Box 34308. Nairobi, Kenya.
- IBFAN Europe Regional Office. GIFA, CP 157, 1211 Geneva 19, Geneva.
- Informative Breastfeeding Service. 16 Gray Street, St. Clair, Port of Spain,
Trinidad.
- Institute for International Studies in National Family Planning. Georgetown
University, Washington, D C 20007, U S A.
- International Baby Food Action Network (IBFAN). 3255 Hennepin Avenue, Suite 230,
Minneapolis. MN 55408, U S A.
- International Organisation of Consumers Unions. Regional Office for Asia and the
Pacific, P O Box 1045. 10830 Penang, Malaysia.
- La Leche League International Inc. 9616 Minneapolis Avenue,
Franklin Park, Illinois 60131, U S A.
- League of Red Cross & Red Crescent Societies. P O Box 372, 1211
Geneva 19, Switzerland.
- Macmillan Press Ltd. Houndmills,
Basingstoke, Hampshire, RG21
2XS, UK.
- Malaysian Breastfeeding Advisory Association. Persatuan Penaishat Penyusuan Ibu
Malaysia, 3rd Floor, 8 JAlan Klyne, Kuala Lumpur 01-21, Malaysia.
- Nursing Mothers' Association of Australia. P O Box 230, Hawthorn, Victoria
3122, Australia.
- Nutrition Center of the Philippines. P O Box 653,
MCC, Makati, Metro-Manila, The
Philippines.
- Oxford University Press. Walton Street, Oxford OX2 6DP, U K.
- Pandora Press. 11 Newfetter Lane, London EC4, UK.
- Singapore Breastfeeding Mothers Group. Consumer Association of Singapore, Trade
Union House Annexe, Shenton Way, Singapore 0106.
- Susu Mamas. P O Box 5857, Boroko, Papua New Guinea.
- Teaching Aids at Low Cost (TALC). P O Box 49, St Albans, Herts AL1 4AX,
UK.
- UNICEF, 3 UN Plaza, New York, NY 10017, U S A.
- World Health Organization (WHO). 20 Avenue
Appia, 1211 Geneva 27,
Switzerland.
BOOKS/ MANUALS
Baumslag, N, 1988. Breastfeeding: passport to life. UNICEF/
NCIH conference - summary of technical papers and general recommendations. NGO Committee
on UNICEF. UNICEF
Huffman, S, and Combest, C, 1988. Breastfeeding: prevention and treatment necessity
for diarrhoea, available in the above and from Center to Prevent Childhood
Malnutrition.
Breastfeeding Information Group. Kenya. How to Breastfeed Your Baby. Ebrahim, G,
J, 1978. Breastfeeding - the biological option. Macmillan Tropical Community Health
Manuals, Macmillan.
Helsing, E, with Savage-King. F, 1982. Breast-feeding in practice: a manual for
health workers. Oxford University Press.
Institute for International Studies in Natural Family Planning: Washington, U S A,
1989. Programmatic guidelines for breastfeeding support and promotion and family
planning and child survival programs.
International Organisation of Consumers Unions & IBFAN. Malaysia, 1985. Protecting
infant health: a health workers' guide to the international code of marketing of breast
milk substitutes.
Kyenkya-Isabirye, M, 1988. Resource directory: recommended materials for training
and advocacy in breastfeeding programmes. Available from: UNICEF: New York, U S A.
League of Red Cross and Red Crescent Societies, Switzerland. Learn more about
breastfeeding and weaning.
Nutrition Center of the Philippines. A manual on infant feeding with emphasis on
breastfeeding.
Palmer, G, 1988. The politics of breastfeeding. Pandora Press.
Savage-King, F, 1985. Helping mothers to breastfeed.
AMREF. Available
from Teaching Aids at Low Cost.
UNICEF, 1985. Bangkok (Regional PSC Officer) Planning a breastfeeding promotion
campaign.
WHO, Division of Family Health Breastfeeding and child spacing - what health
workers need to know. AUDIOVISUALS Series of slides (200) on infant feeding with emphasis on breastfeeding. Nutrition
Center of the Philippines.
Series of slides with script - Breast feeding. Describes advantages to mother and
infant, also the prevention and management of common difficulties. Teaching Aids at Low
Cost.
Series of slides with script - Breast feeding problems: the common problems of
breastfeeding, and how to overcome them. Teaching Aids at Low Cost. NEWSLETTERS TIBS News. Informative Breastfeeding Service. Bi-monthly in English. Free.
Mothers and Children. Bulletin on infant feeding and maternal nutrition.
Clearinghouse on Infant Feeding & Maternal Nutrition, American Public Health
Association. Quarterly in English. French and Spanish. Free to developing countries.
Breast Briefs. Geneva Infant Feeding Association (GIFA), Switzerland.
IBFAN Africa News. IBFAN Africa. Published in English and French.
IBFAN Action News. IBFAN U S A. Ten issues per year in English. Free to
developing countries.
|
Acknowledgement The information in the insert has been taken from a range of
sources. We would especially like to thank Dr. Felicity Savage for her generous help and
advice. Line drawings by Sara Kiunga-Kamau and Ivanson Kayaii, from 'Helping Mothers
to Breastfeed' by Dr Felicity Savage.
|
Breastfeeding
Health Basics - A supplement to Issue no. 37 June 1989
Page Navigation
This edition of Dialogue on Diarrhoea Online is produced by Rehydration Project. Dialogue on Diarrhoea was published four times a year in English, Chinese, French, Portuguese, Spanish, Tamil,
English/Urdu and Vietnamese and reached more than a quarter of a million readers worldwide. The English edition of Dialogue on Diarrhoea was produced and distributed by Healthlink Worldwide. Healthlink Worldwide is committed to strengthening primary health care and
community-based rehabilitation in the South by maximising the use and impact
of information, providing training and resources, and actively supporting
the capacity building of partner organisations. - ISSN 0950-0235 Reproducing articles
Healthlink Worldwide encourages the reproduction of
articles in this newsletter for non-profit making and educational uses. Please
clearly credit Healthlink Worldwide as the source and, if possible, send us a copy of any uses made of the material.
|
updated: 4 March, 2016
|
version of this Issue